What are the causes of peripheral vascular disease?
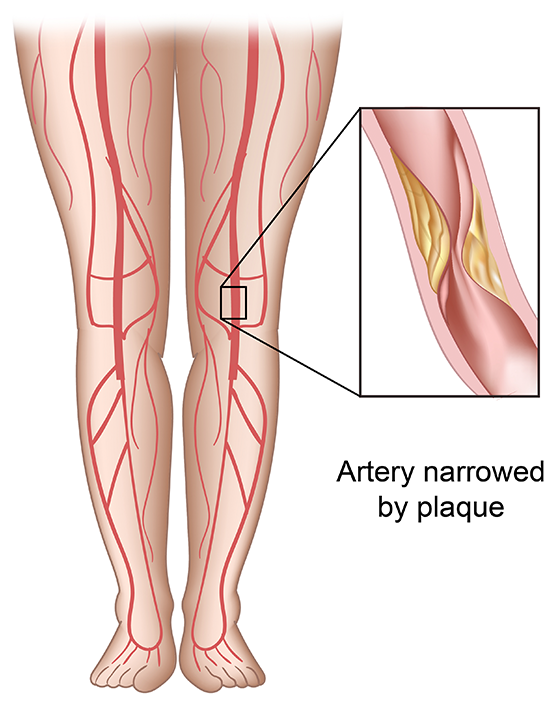
Peripheral vascular disease or PAD may commonly occur in the arteries of the legs. PAD occurs when plaque builds up obstructing the flow of blood to the legs. This plaque buildup may be caused by several risk factors for blood vessel disease. Family history is an important component, as is smoking cigarettes, high cholesterol, high blood pressure, and diabetes.
What are the symptoms of PAD?
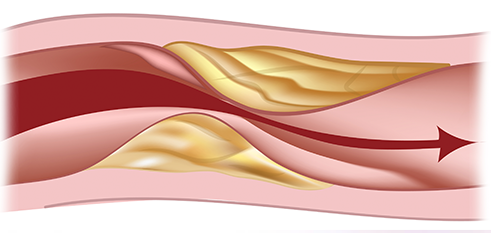
PAD may cause pain in the muscles of the legs when walking because the muscles are not receiving adequate oxygen. These symptoms may be worse when walking uphill or rapidly and are usually relieved with rest. Patients with severe multilevel blockages may have pain continually and worse when they sleep, in the legs due to severe lack of circulation. This may be worse at night because the legs are elevated. Patients with severe disease may also have non healing wounds or gangrene.
What are the tests used to diagnose PAD?
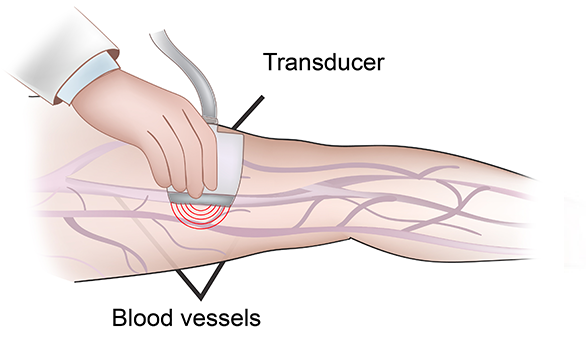
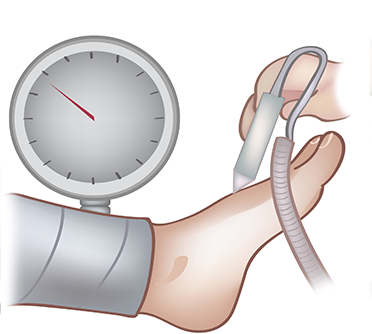
If you have symptoms suggestive of PAD, your physician will first order an arterial ultrasound exam. This non-invasive exam allows determines the location and severity of the blockage. Measurement of pressures at the ankle and at the toes will also help determine how severe the overall blockage is. If treatment is needed, your physician will likely need to perform a test with contrast to better image the arteries. This may be done with either a CT scan, MRI or angiogram. During angiography, dye is directly injected through a small puncture site in the leg artery in the groin area to visualize the area of blockage. If the blockage is suitable for percutaneous treatment, angioplasty, stent or atherectomy may be performed to improve the blood flow to the leg.
What are the treatments for PAD?
First and vitally important is that all risk factors for PAD should be treated. This means smoking must be stopped, and cholesterol, diabetes and high blood pressure should bel well controlled. Without controlling these risk factors, the treatment that is performed to restore blood flow may not be durable.
For patients who have pain with walking but no pain at rest, ulcer or gangrene, a trial of exercise therapy with risk factor modification may be advised. Patients will be asked to walk at least 5 times a week for 30 minutes. Walking should be done to the point of muscle pain and then continued for a short period as tolerated. Patients should then rest until the pain resolves and then begin walking again. This will encourage new blood vessel formation and often will greatly improve the walking distance so that procedures are not required. The exercise therapy may be accompanied with a medication called pletal which can dilate blood vessels and improve walking distance.
For patients who fail exercise therapy and are disabled by their leg pain a procedure may be required to improve blood flow. Similarly if a patient has severe disease with pain at rest or non- healing wounds a procedure will likely be needed.
If the blockages are relatively short, they may be treated with an angioplasty or stent placement. This is done through the insertion of a small flexible tube in the femoral artery in the groin. Through this insertion site, we can place a balloon to dilate the artery and if needed a stent to hold it open improving the blood flow. The recovery from these procedures is rapid and they may even be done as an outpatient in the office depending on the circumstances. If the blockages are longer, it may not be possible to treat it with stenting. In these circumstances a bypass surgery may be required in the hospital. This surgery usually requires several days in the hospital and a longer recuperation time.
Unfortunately peripheral vascular disease cannot be "cured" by a procedure. Although blockages may be stented or bypassed they can recur and even become worse. It is therefore very important to follow up with your surgeon regularly. Depending on your procedure, ultrasounds may be requested periodically to evaluate the vessels to ensure that the repair remains durable. Continued optimization of all risk factors is a critical component to success and cannot be emphasized enough.