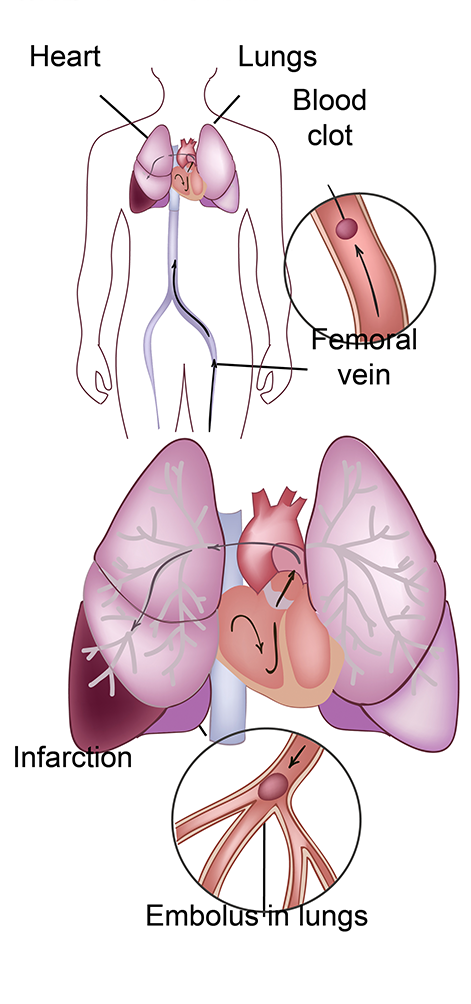
What is a pulmonary embolus?
A pulmonary embolus or PE is a blood clot which blocks the flow of blood through the lung and therefore prevents that portion of the blood from getting oxygen from the lung
How does a pulmonary embolus occur?
The blood clot usually travels to the lungs from another part of the body, most commonly from the legs, but it could also occur from the upper extremities. Please see our discussion of DVT to see how and why these clots may form.
What are they symptoms of a pulmonary embolus?
A smaller pulmonary embolus may cause chest pain, cough which may produce bloody sputum, shortness of breath and rapid heart rate. In addition to these symptoms a large PE may cause dizziness or fainting and can be fatal.
How are PEs diagnosed?
A CT scan of the chest with IV contrast is the main method. This allows us to see the pulmonary arteries and visualize the clots within them. We can determine the size and location of the PE. If a patient has kidney disease they may not be able to receive IV contrast. In this case, a ventilation perfusion scan can be performed in the nuclear medicine department without the need for contrast. This test is not quite as accurate as the CT scan but is also very effective. Once the diagnosis is confirmed an ultrasound of the lower extremities is done to look for the source of the PE. If the PE is large an echo test of heart may be done to assess how much strain there is on the heart from the embolus.
How are PEs treated?
Anticoagulation is the hallmark for treatment. The options are very similar to what we outlined in our section on DVT and the reader is referred there. If the pulmonary embolus is very large and the patient has low blood pressure, severe difficulty breathing, or excessive strain on the heart, then more aggressive measures may be considered. In these cases an active clot dissolving medicine can be administered through an IV. Unlike the anticoagulants which stabilize the clot and allow the body to dissolve it gradually, the active clot dissolving medications called thrombolytics break down the clot immediately. These medications do have the risk of serious bleeding and are only used when the life of the patient is at risk. Your surgeon may also elect to place a small catheter within the pulmonary vessels to suction or break up some of the clot. This procedure can be done in conjunction with or in place of the thrombolytics and is reserved for cases where the patient is gravely ill.
How long do I need to be treated with anticoagulation?
For a pulmonary embolus that has a cause such as a long flight or surgery, the normal duration of anticoagulation is 6 months
If there is no clear cause and the pulmonary embolus is "unprovoked" then indefinite treatment may be needed. In these cases, hematology referral is important to search for conditions that may cause problems with clotting such as a genetic disorder of clotting, autoimmune disease, or a malignancy.
What if I cannot receive anticoagulation?
If a patient has a DVT of the lower extremities and a PE and cannot receive anticoagulation due to bleeding then an inferior vena caval filter (IVC filter) is indicated to prevent additional embolism to the lungs. The filter is able to trap clots from the legs before they reach the lungs. Filters do have small long term risks but they can be lifesaving when used appropriately.